Hey Man! You had lab results back? You have low testosterone? Are you considering testosterone replacement therapy (TRT)?! Thinking about what formulation is best ? How much does it cost? If you are weighing the benefits of testosterone pellet therapy vs. injection therapy, We’ve got your back!
In this article, we describe the pros and cons of exogenous injectable T and subdermal pellets to help you be well-informed before making the decision with your doctor when it comes to choosing the best formulation of testosterone hormone therapy. Testosterone Pellets vs Injections, let’s go!
Key Takeaways
- Each testosterone therapy formulation comes with its own advantages and drawbacks.
- You need to discuss with your doctor the best formulation that fits you the most.
- T Enanthate is the cheapest among all injectable testosterone.
- Testosterone pellets are more expensive than testosterone replacement therapy injections
- Testosterone pellets need minor surgical procedure to be implanted.
- Pellets may be associated with local pain, irritation and inflammation at the insertion site.
Testosterone
Testosterone is an essential, vital sex hormone for males, required for differentiation, and developmental growth. [9]
In young, healthy men (20 – 30 years old), the normal levels of serum T (400 – 700 ng/dL) are controlled by the feedforward and feedback components of the hypothalamic-pituitary-gonadal axis and are maintained within the normal range of 300–800 ng/dL. [9]
Several studies have shown that Serum testosterone (T) levels decline gradually with age in men after the third decade of life at an approximate rate of 1-2% per year, varying from one to another, and are affected by several factors such as adiposity and chronic diseases. [9]
When Do You Need To Start Testosterone Replacement Therapy?
Hypogonadism in men is the clinical syndrome that results from failure of the testis to produce enough testosterone and sperm cells. [3]
In 2018, the American Urological Association recommended the use of testosterone therapy in patients with total testosterone < 300 ng/dl. [9]
Here is a list of the most common symptoms and signs of low testosterone:
- Anemia.
- Depressed mood.
- Erectile dysfunction.
- Decreased libido and sexual function.
- Reduced muscle mass and strength.
- Reduced bone mass and osteoporosis.
- Insomnia, decreased energy levels and weight gain.
- Forgetfulness, difficulty in concentration, and loss of memory.

Testosterone Replacement Therapies
Testosterone Pellets
Numerous T formulations are Food and Drug Administration (FDA) approved in the United States for the treatment of hypogonadism. [1]
Several commonly used T formulations include injectables, transdermal gels, and implantable subdermal pellets. [1]
Beyond gels, patches and injections, another option for testosterone replacement are the subdermal implants. [2]
Testosterone pellet were among the first modalities applied for testosterone therapy, reaching back to the late 1930s. [4]
A review of 973 implantations in 221 men showed adverse local effects such as extrusion, bleeding and inflammations/ infections in 11%. [4]

Pharmacokinetic Evaluation and Dosing of Subcutaneous Testosterone Pellets
Modern pellets are produced by high-temperature moulding. [4]
They are available in two sizes, containing 100 or 200 mg of crystalline steroid, with a length of 6 or 12 mm and a common diameter of 4.5 mm. [4]
If 3-6 implants are inserted, slowly declining serum T levels in the normal range are achieved for 4-6 months. [4]
There is, however, an initial burst release, so that supraphysiological levels of about 50 nmol/L result. [4]
Within the first weeks of application, serum T concentrations increase to very high levels and then decline steadily into the hypogonadal range. [5]
The overall terminal half-life was calculated at 71 days. [4]
Three 200-mg or six 100-mg pellets maintain their effectiveness for up to half a year. [5]
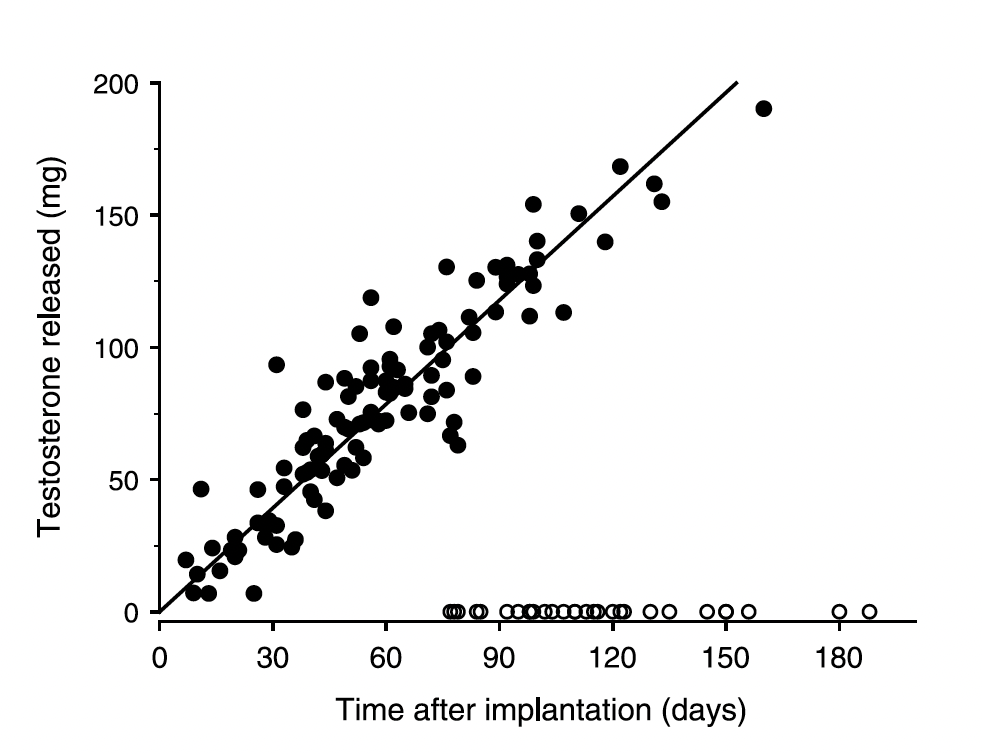
Each 200 mg testosterone pellet releases 1·3 mg testosterone per day. Assuming a constant daily T release until complete dissolution, this provides a crude estimate that four testosterone pellets should last ∼154 days following implantation. [6]
The standard dose of four 200 mg pellets releasing an estimated 5·2 mg testosterone per day, a figure quite consistent with the best available estimates of endogenous T production rate for eugonadal men of 5–7 mg per day using tritiated or stable isotope tracers. [6]
Previous studies of testosterone pellet implants have clearly established that circulating testosterone levels rise rapidly into the physiological range where they are maintained at stable levels from day to day for months before gradual decrease to pretreatment levels between 4 and 7 months, depending upon dose, after implantation as pellets undergo full absorption. [6]
How To Implant?
They are administered in a 10- to 15-minute procedure in the office every three to six months depending on follow-up laboratory results. [2]
Implanted by a tunnelling technique using a trocar, they remain under the skin of the lower abdominal wall and are totally biodegradable. [4]
Injectable T formulations are associated with significant increases in the risk of erythrocytosis relative to testosterone gels and pellets, possibly related to elevated mean or peak testosterone levels. [1]
Pros
Patients do not have to self-inject or apply gels repeatedly. [2]
The extended release decreases the ‘up and down’ feelings often experienced with the intramuscular injections. [2]
Cons
The need for regular office visits.
The pellets require minor surgery for insertion. [5]
Possible pain, irritation and bruising at the site of insertion.
An inflammatory process often accompanies extrusion. [6]
Minimal risk of infection.
Monitoring
Measure testosterone levels at the end of the dosing interval. [3]
Adjust the number of pellets and/or the dosing interval to achieve normal testosterone level [3]
When To Call for Reimplantation?
Patients are routinely encouraged at the time of implantation to make phone contact as soon as they re-experienced their familiar symptoms to book a re-implantation. [6]
Long-acting Intramuscular Testosterone
Long-acting intramuscular (IM) injections of T esters, such as T enanthate, T cypionate and a mixture of esters have been used for many years for the treatment of hypogonadism.
Testosterone Undecanoate
An extra long-acting injectable form of T undecanoate in castor oil, with even longer half-life of about 34 days, that allows increased dosing intervals of up to three months.
It needs to be administered with an initial dose of 750 mg, followed 4 weeks later by another 750 mg dose. This is then followed by an intramuscular injection once every 10 weeks.
Individual intervals are determined according to serum T levels which are measured immediately before the next injection.
Values that are too high lead to extension of injection intervals, those that are too low to a shortening in injection intervals.
Slow intragluteal injections are recommended.
Pros
The achievement of relatively stable normal T levels.
The least frequent dosing among IM preparations.
The recent IPASS study demonstrated that injectable TU was effective and well tolerated with marked improvements in several psychosexual functions and waist circumference.
Cons
The relatively long wash-out period which may cause problems if complications appear.
Higher cost compared to other IM formulations.
The risk of pulmonary oil microembolism (POME) and anaphylaxis.
Needs to be administered in the office as a slow injection over 2 minutes.
Patients need to be monitored for 30 to 45 minutes after administration due to the risk of developing pulmonary oil microembolism.
Testosterone Enanthate
Testosterone enanthate has been the most common preparation for T substitution since its introduction in the early 1950s. [7]
It has a terminal half-life of 4.5 days. Its maximum concentrations are reached after 10 h following a single injection of 250 mg. [7]
Multiple-dose pharmacokinetics reveal an optimal injection interval of 2-3 weeks at a dose of 200-250 mg. [7]
Pros
- The main advantages of these formulations, especially T enanthate, are the effectiveness in initiating and maintaining normal virilization in all hypogonadal men.
- Freedom from daily administration.
- Low cost.
Cons
- The need for deep IM injection every 1–3 weeks.
- Fluctuations in serum T levels resulting in fluctuations in energy, mood and libido in many patients. These fluctuations are more pronounced when dosing interval is increased.
Testosterone Cypionate and Testosterone Cyclohexanecarboxylate
T cypionate and T cyclohexanecarboxylate resemble the pharmacokinetic properties of T enanthate. [7]
They do not provide an advantage over the enanthate ester.
Testosterone Propionate
T propionate has a terminal half-life of only 19 h. After a single injection of 50 mg, maximum concentration is reached after 14 h. It requires frequent injection. [7]
Multiple-dose pharmacokinetics reveal optimal intervals of 2-3 days, but fluctuations below normal-range values persist. Therefore, it is not suitable for long-term treatment of hypogonadism. [7]
Adverse Effects of Injectable Testosterone
Cardiovascular Events
In a retrospective analysis of three databases, use of injectable preparations was associated with a greater risk of MI and stroke when compared with T gel use.
Erythrocytosis
Erythrocytosis is a common adverse effect of T administration, particularly with T ester injections and in older men.
Erythrocytosis also occurred significantly earlier in men on injectable T formulations when compared with the testosterone pellets.
pulmonary oil microembolism (POME)
Although the injectable preparations are generally considered very safe, there is a risk of pulmonary oil microembolism (POME).
It’s clinically characterized by brief respiratory symptoms such as cough, urge to cough and dyspnea immediately after the injection.
It has been observed after injection of T enanthate in castor oil at a rate of 1.5% of injections. Similarly, it may occur after intramuscular injection of T undecanoate, although at a much lower rate.
The FDA has required a special warning of POME when licensing intramuscular T undecanoate (Aveed®) in the USA. This preparation contains only 750 mg T undecanoate and therefore requires slightly shorter injection intervals of about 10 weeks. [8]
Monitoring
Injectable T enanthate or cypionate: measure serum T level midway between injections. If T is 700 ng/dl (24.5 nmol/liter) or 400 ng/dl (14.1 nmol/liter), adjust dose or frequency. [9]
Injectable T undecanoate: measure serum testosterone level just prior to each subsequent injection and adjust the dosing interval to maintain serum T in mid-normal range.
Cost of Testosterone Replacement Therapy
Pellets
The cost of testosterone pellet insertion varies. Typically, patients will generally pay $650-750 for a single pellet inserion procedure, depending on the dose and the number of pellets required.
Your practitioner only needs to insert pellets 2 to 4 times a year, depending on how rapidly your body responds to testosterone.
Injections
In general, Injections are the most affordable TRT option. Without insurance coverage, the cost of a single 200 mg/mL testosterone vial can range between $40 and $100 a month. [10]
In Conclusion
When it comes to testosterone replacement therapy (TRT), the choice between T injections and pellets isn’t one-size-fits-all. Each method effectively addresses low testosterone symptoms, but the best option depends on your unique needs.
Both injections and pellets come with their own advantages. Injections offer flexible dosing, while pellets provide a steady, long-term release. The key is to weigh the pros and cons of each option carefully.
Before making a decision, be informed about what each treatment involves. We highly recommend consulting your doctor to discuss what aligns best with your health goals and lifestyle. Ultimately, finding the right TRT method is about personalizing the approach to suit you best.
Skip Ahead
Toggle