Recently you have been experiencing mood changes, low libido, and decreased sexual function. You checked your testosterone levels and found out that they are low. Now, you want to start testosterone replacement therapy but oh, shit. This may impact my sperm production..
I won’t be able to have kids. Should I start? Should not? What are my options? What should I do? You are confused? Have a lot of questions? Don’t know what to do? Here you go!
We’ve got your back. In this article, we gather all the information you need on How To Increase Sperm Count While On TRT.
Key Takeaways
- Men of reproductive age with low testosterone should be counseled on the adverse effects of TRT on fertility
- Obtaining a semen analysis and possible cryopreservation of sperm should be offered if TRT is prescribed to men interested in preserving fertility
- Options such as clomiphene citrate and hCG along with a referral to a reproductive urologist should be considered to naturally increase testosterone levels in those men with low testosterone who want to avoid TRT
What Is Testosterone?
Testosterone is an essential, vital sex hormone for males, required for differentiation, developmental growth, and phenotype maintenance. [3]
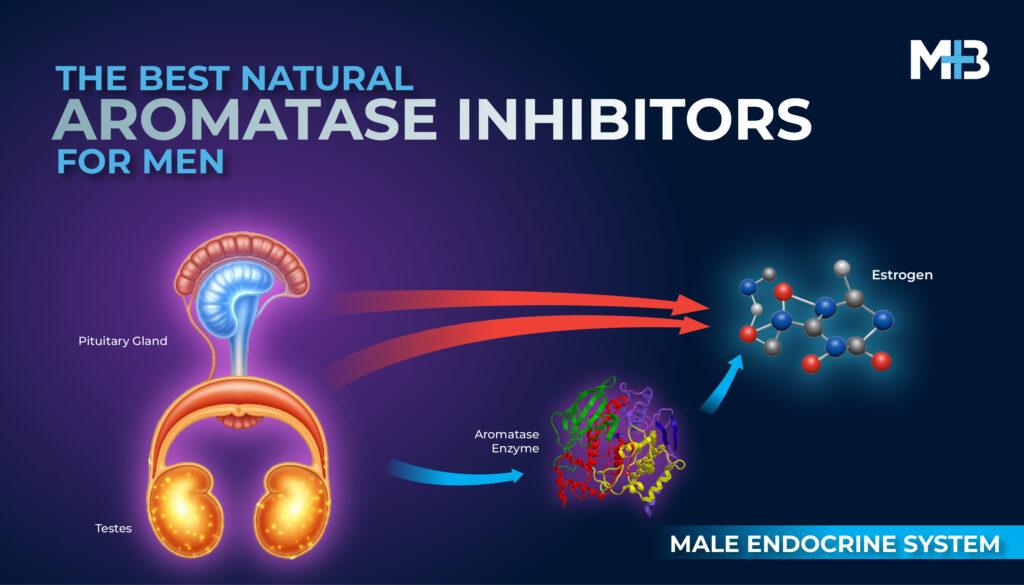
The levels of testosterone are regulated by the hypothalamic-pituitary-gonadal axis. [3] Every 90 min, the hypothalamic pulse generator secretes gonadotropin-releasing hormone (GnRH) into the hypothalamic-pituitary system, with subsequent release of luteinizing hormone (LH), which in turn stimulates the Leydig cells in the testes to produce testosterone. [3]
Only about 2% of total testosterone circulates in the free form, while the remaining 98% is tightly bound to sex hormone binding globulin or albumin.
Albumin binding is weak, and most of that fraction of testosterone is eventually bioavailable and can be measured and reported as bioavailable testosterone.
What Are The Normal Levels of Testosterone?
In young, healthy men (20 – 30 years old), the normal levels of serum testosterone (400 – 700 ng/dL) are controlled by the feedforward and feedback components of the hypothalamic-pituitary-gonadal axis and are maintained within the normal range of 300–800 ng/dL. [3]
Testosterone and Fertility
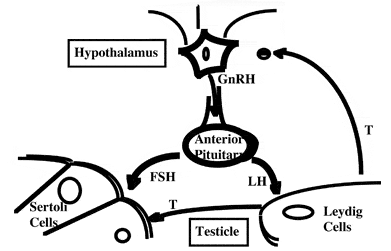
In healthy adult men, testosterone production is precisely regulated by the HPG axis. Higher cortical centers in the brain signal the hypothalamus to secrete gonadotropin-releasing hormone (GnRH) in a pulsatile fashion. [5]
GnRH in turn stimulates the release of LH and FSH from the anterior pituitary which modulates testosterone production from the Leydig cells and spermatogenesis by the Sertoli cells, respectively. [5]
Spermatogenesis is largely dependent on the action of FSH on Sertoli cells coupled with high intra-testicular testosterone concentrations. [5]
Within the seminiferous tubules, only Sertoli cells possess receptors for both FSH and testosterone. Numerous signaling pathways are activated when FSH binds to FSH receptors on these cells. [5]
Intra-testicular testosterone is required in spermatogenesis for the formation of the blood-testis barrier (BTB). [5]
Testosterone is also required in maintaining connections between Sertoli cells and the haploid spermatid germ cells. [5]
Testosterone aids in this process and increases the efficiency of germ cell attachment to Sertoli cells. Testosterone is also essential for the release of mature spermatozoa from Sertoli cells. [5]
Low Testosterone
Several studies have shown that Serum testosterone levels decline gradually with age in men after the third decade of life at an approximate rate of 1-2% per year, varying from one to another, and are affected by several factors such as adiposity and chronic diseases. [3]
Previous studies have shown that the declining function in older men is related to bioavailable testosterone levels. Therefore, Testosterone replacement therapy (TRT) is proposed as an intervention to improve the health span of older men.
In 2018, the American Urological Association recommended the use of TRT in patients with total testosterone < 300 ng/dl. [4]
Prevalence of Testosterone Deficiency
In the United States, the prevalence of testosterone deficiency is approximately 40% in men aged 45 years and older. [1]
A large international web survey using the Aging Males’ Symptoms (AMS) questionnaire showed that 80% of men aged 16-89 years (mean age 52 years) have symptoms suggesting testosterone deficiency. [2]
Surprisingly, 40% of the respondents to this survey were at younger ages. [2]
While testosterone replacement therapy (TRT) confers great benefits to men with low testosterone levels and symptoms of testosterone deficiency, it also comes with some side-effects such as infertility which may concern men who wish to have children in the future.
Many testosterone users and even some clinicians are unaware that exogenous testosterone suppresses the hypothalamic-pituitary-gonadal (HPG) axis and may result in infertility. However, the good news is, in most cases, TRT induced infertility is reversible.
So, in this article, we will give you some information about how can you manage your low testosterone levels and minimize the risk of infertility while on TRT.
TRT and Testosterone Deficiency
Testosterone is currently approved by the Food and Drug Administration (FDA) for primary or secondary hypogonadism. With the worldwide increase in men’s life expectancy and the development of proper testosterone preparations, the interest in prescribing TRT has dramatically increased.
The use of testosterone replacement therapy (TRT) among men over the age of 40 years has increased more than 3-fold over the last decade. [5]
TRT is used to treatment late-onset hypogonadism (LOH) – a common proplem in aging men and is associated with testosterone deficiency.
Symptoms of testosterone deficiency include anemia, depressed mood, erectile dysfunction, decreased libido and sexual desire, reduced muscle mass and strength, reduced bone mass and osteoporosis, insomnia and a reduced sense of general well-being, forgetfulness, difficulty in concentration, and loss of memory.
The Endocrine Society and American Urological Association (AUA) recommends treating symptomatic men with low testosterone documented on two morning fasting serum total testosterone concentrations. [5]
Does TRT Decrease Your Sperm Count?
Exogenous testosterone comes in various preparations and each form carries various risks. Along with an increase in hematocrit, a major adverse effect of TRT is the diminished sperm production because of the decreased intra-testicular concentration of testosterone and suppression of the hypothalamic-pituitary-gonadal (HPG) axis. [5]
As testosterone levels increase, negative feedback suppression is exerted on the androgen receptors in the hypothalamic neurons and pituitary gland, thereby inhibiting the release of GnRH, FSH and LH. [5]
The exogenous administration of testosterone suppresses the release of gonadotropins (FSH and LH) to levels below that required for spermatogenesis. [5]
Suppression of follicle stimulating hormone (FSH) release from the pituitary gland impairs sperm production and suppression of luteinizing hormone (LH) release inhibits intra-testicular testosterone production. [5]
The inhibition of LH release by exogenous testosterone leads to the suppression of endogenous testosterone production by the Leydig cells. [5]
The decreased intra-testicular testosterone combined with the suppression of FSH leads to decreased germ cell survival and maturation. [5]
The low intra-testicular testosterone results in decreased proliferation of spermatogonia, defects in spermiation of mature spermatozoa by Sertoli cells and accelerated apoptosis of spermatozoa. [5]
Since 80% of testicular volume consists of germinal epithelium and seminiferous tubules, a reduction in these cells is usually manifested by testicular atrophy and this reflects the loss of both spermatogenesis and Leydig cell function. [5]
Despite the androgenic effects of testosterone on sexual function, libido and mood; its effect on gonadotropins leads to the inhibition of sperm production. [5]
The Endocrine Society and American Urological Association (AUA)recommend against the use of testosterone for treatment of hypogonadism in men who desire fertility in the next 6 to 12 months. [5]
Do Testosterone Injections Kill Sperm Count?
In a Chinese study of a monthly intramuscular TU injection, an azoospermia rate of 93% to 98% was achieved after 6 months with 1 million/mL as the criteria for effective suppression in this study. [6]
Two studies by the World Health Organization (WHO) Task Force on Methods for the Regulation of Male Fertility found an azoospermia rate of 64% to 75% in 6 months with testosterone enanthate. A sperm concentration of 3 million/mL was used as a threshold for effective suppression of spermatogenesis in this study. [7,8]
These studies confirm the ability of testosterone replacement therapy to decrease sperm count and provide evidence that men who desire fertility should not be prescribed TRT.
TRT and Infertility
Discuss Fertility Before Starting Testosterone Therapy
Clinicians must address male infertility risks when considering testosterone replacement therapy (TRT) for patients desiring children.
Many patients are surprised to learn testosterone may suppress fertility despite boosting libido and erectile function.
It’s crucial to thoroughly discuss the patient’s fertility goals before initiating TRT to avoid future complications.
This conversation should also explore long-term fertility plans, helping the doctor align treatment with the patient’s reproductive goals.
By balancing hypogonadism symptom relief with fertility preservation, physicians can tailor treatments to meet both immediate and future needs effectively.
Semen analysis and Blood Tests
Physicians should also educate men already on TRT. There has been an increase in TRT use among men aged 18 to 45 years and more than 20% of these men did not get a baseline testosterone level prior to initiation of TRT. [14]
Some of these men may not know about its effects on fertility and may not have discussed it with their prescribing physician.
This study also showed that less than 2% of men on TRT obtained a baseline semen analysis. In addition to the routine serum total testosterone, LH, and hematocrit prior to starting TRT, every man of reproductive age should have a baseline semen analysis. [14]
The baseline semen analysis will identify men with a decreased baseline sperm count, as a reference value for future semen analyses after TRT use.
How Quickly Does TRT Impact Fertility?
Previous study reported that exogenous testosterone can suppress spermatogenesis and lead to azoospermia in 65% of normospermic men within 4 months of use. [7]
However, it is important to know that every body’s response to TRT is different. So, some men may experience quick decline in sperm production while others may experience gradual decline.
It all depends on how well—and fast—the body responds to the additional exogenous testosterone.
Is the Impact of TRT On Fertility Permanent?
In most cases, TRT-induced infertility is not permanent. When TRT is stopped under medical supervision, infertility usually be reversible especially if TRT was only for short-term.
However, for a very small percentage of men, fertility doesn’t return after stopping TRT.
How Long After Stopping TRT Does Your Sperm Count Increase?
Cessation of exogenous testosterone will lead to the reversal of TRT-induced azoospermia in 64% to 84% of men with a median time of about 110 days. [7,9]
Azoospermia or severe oligospermia may be seen in these patients, but most men should return to baseline semen analyses in 6 to 9 months after cessation of TRT. [7,9]
All men in these studies recovered to baseline levels after cessation of therapy; however, it took up to 2 years for some men to recover. [7,9]
A 2006 integrated analysis showed that 90% of patients were expected to return to baseline sperm concentration values 12 months after cessation of treatment and 100% after 24 months.
Kohn et al studied spermatogenesis recovery with human chorionic gonadotropin (hCG) and selective estrogen receptor modulators (SERM) in men with infertility associated with TRT use. [10]
In this study, only 30% men were not able to achieve a total motile sperm count of more than 5 million after 12 months in the study. [10]
They found that the failure of recovery is associated with older patients and longer TRT duration. [10]
An older man who was on TRT for a longer time can expect a longer sperm recovery time frame than a younger one who was on TRT for a shorter period of time.
If You Want To Be A Father and You Are On TRT, What Should You Do?
Talk to your doctor. Your doctor will be able to help you determine whether your low testosterone can be normalized by TRT or by alternate treatment option.
For example, there could be a problem with your pituitary gland, in which case pituitary hormone supplementation or another prescription medication could be enough to rectify the low testosterone levels while leaving your sperm production unaffected.
If You’re On TRT and You Want To Be a Dad, Should You Stop?
You should never stop TRT on your own. You should never stop TRT suddenly. If you are on TRT and you have a desire to be a father. Talk to your doctor and ask for guidence.
If your doctor determines that stopping TRT is the best course of action because of concerns about TRT and fertility, he may start withdrawing your doses gradually, or consider alternative medications such as clomid to help speed up the increase in sperm count again.
How Can You Increase Sperm Count While in Need for TRT?
You have low testosterone and you want to be a biological father in the future? You have concerns about the impacts of TRT on your sperm count? We have your back!
Here are some of the suggested alternative options for you. However, as we usually say, what works for you does not necessarly work for others. So, usually consult with your doctor first before making any decision.
Human Chorionic Gonadotropin (hCG)
Although the exact mechanism of action and production site in males are not fully understood, it is known that hCG mimics the effects of LH and stimulates the Leydig cells in the testicles to produce endogenous testosterone. [5]
Evidence in a 2015 study of 49 men showed that 3,000 units of hCG subcutaneously every other day is effective in supporting the recovery of spermatogenesis without significant adverse effects. [5]
Several studies have shown that low-dose hCG can be used with TRT to maintain high levels of intratesticular testosterone while men are being treated for hypogonadism. [5]
While hCG is effective in increasing testosterone, various studies have shown that it is also efficacious in inducing spermatogenesis. [5]
It is even effective in helping with the recovery of spermatogenesis in men who were on TRT.
Clinicians generally agree on using 2,000 IU of hCG administered subcutaneously 3 times per week as defined by the 2002 American Association of Clinical Endocrinologists guidelines.
Clomiphene Citrate
Clomiphene citrate is a selective estrogen receptor modulator. It has been primarily used for infertility treatment in both genders for over 50 years. [11]
It selectively blocks estrogen receptors in the hypothalamus and pituitary, thereby increasing gonadotropin-releasing hormone, luteinizing hormone, and follicle-stimulating hormone release. This boosts endogenous testosterone levels. [11]
A previous study reported that clomiphene achieved testosterone levels comparable to those of testosterone gels. [12]
Another study found that clomiphene significantly increased testosterone levels without changing prostate-specific antigen or hematocrit values. [13]
Clomiphene is a less expensive alternative to testosterone replacement with the added benefit on fertility. [11]
Adjunctive hCG and Clomiphene
Adjunctive hCG and clomiphene can be used with TRT to maintain testicular size and intra-testicular testosterone concentrations. [5]
Talk To a Specialist
Referral to a reproductive urologist should be considered in a male with low testosterone interested in fertility. [5]
Consider Sperm Freezing
If you’ve been diagnosed with low testosterone and you want to have children in the future, the best thing you can do to protect your fertility options is to freeze some sperm.
Sperm freezing is the process of using liquid nitrogen to preserve one or more sperm samples for possible use later on.
It’s a fairly simple process. First, you produce a semen sample. This sample is then assessed under a microscope (semen analysis) to determine if your sperms are healthy and viable for freezing.
Finally, sperm are plunged into liquid nitrogen to freeze them at a temperature of -196ºC — the temperature at which biological activity pauses — and transferred to liquid nitrogen storage tanks to maintain their low temperature.
Once frozen, your sperm can be stored indefinitely without a decrease in quality or likelihood that it will create a pregnancy.
Frozen sperm can be used in intrauterine insemination (IUI) and IVF, a process in which eggs and sperm are combined outside the body in a lab.
Skip Ahead
Toggle