Believe it or not, men naturally have some Estrogen in their bodies, but too much can be detrimental, potentially causing issues like water retention or even Gynecomastia (Gyno). So, what is the best way to control estradiol on TRT?
Most men think of estrogen as an exclusively female hormone, but that’s not the case. Testosterone is the precursor of estradiol, an estrogen, and the primary female sex hormone.
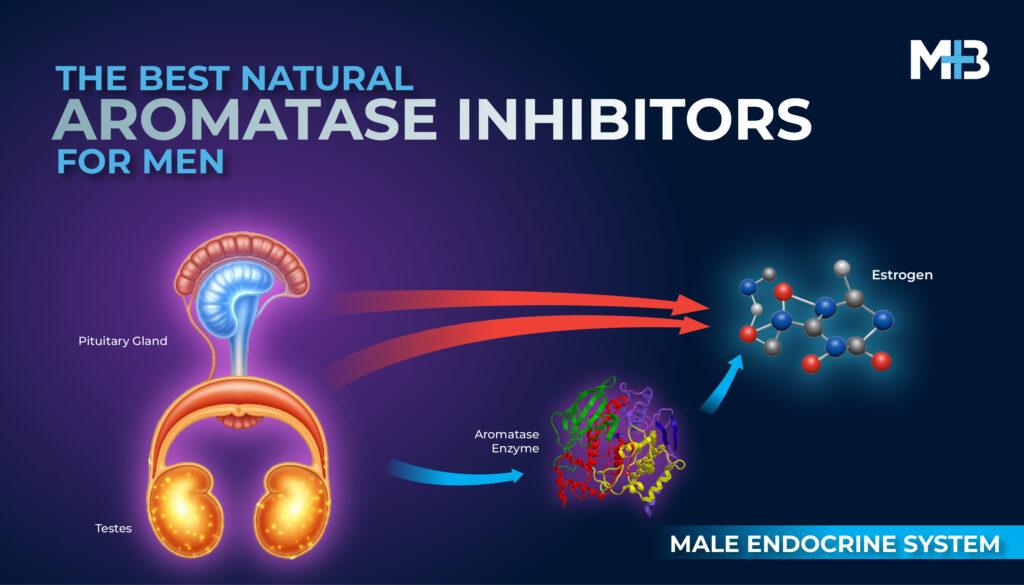
Testosterone is converted into estradiol via the aromatase enzyme and therefore being on testosterone replacement therapy (TRT) can potentially elevate estrogen levels.
Fortunately, most men on standard TRT dosages do not experience high estradiol levels. Nevertheless, genetically predisposed men may experience symptoms associated with high levels, which may lead to certain unwanted side effects.
Want to know more on the Best Way To Control Estradiol On TRT? Here you go…
Key Points
- TRT can increase estradiol (E2) because testosterone converts to estrogen via the aromatase enzyme 💪
- High E2 isn’t common on standard TRT but can cause side effects like water retention or gyno in susceptible men 💧
- Monitoring symptoms and getting blood tests are key to understanding your individual E2 response 🩸
- Aromatase inhibitors (AIs) like Anastrozole are effective estrogen blocker options if needed, but require careful management 💊
- Lifestyle factors like managing body fat can significantly impact aromatization and E2 levels naturally 🔥
What is Estrogen?
While estrogens are defined by their feminizing effects, they are found in both genders. Estrogen is a hormone that is not only prevalent in females but also plays an important role in male physiology. [1]
Estrogens have been known to be present in substantial concentrations in men for several decades, yet their role in male physiology remains an area of considerable uncertainty and controversy. [1]
Because of the increased interest in testosterone (T) deficiency and testosterone replacement therapy (TRT), there has been renewed interest in estrogens, particularly their role in sexual function. [1]
It is well known that men on testosterone replacement therapy will have a corresponding rise in their estrogen level. Therefore, Monitoring and managing estrogen levels are paramount to optimizing testosterone therapy results. [1]
Estrogen has long been known as an important hormone for bone and vascular health in both males and females, but its role in sexual function, erectile function, sex drive, weight loss, and performance are becoming more investigated. [1]
In men on Testosterone replacement therapy who look to optimize performance, sex drive, muscle growth, and weight loss, estrogen management must also be a component of therapy. [1]
Testosterone and estrogen are strongly linked, as testosterone is a major source of estradiol (E2) via aromatization. [1]
Endogenous estrogens in humans are found as estrone (E1), 17b-estradiol (E2), and estriol (E3).

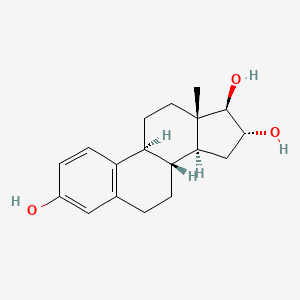
Of all known estrogens, E2 has the highest affinity for the estrogen receptors (ERs) and is the most biologically active. [2]
Estrogen Production In Men
In men, E2 is primarily produced via peripheral aromatization of serum testosterone. However, about 20% of serum E2 in men is produced by Leydig cells in the testes. [1]
A small amount comes from the conversion of other androgens. [3].
As with testosterone, a substantial fraction of E2 is bound to sex-hormone binding globulin (SHBG) and this fraction is not considered to be biologically active. [1]
Factors Affecting Estrogen Production In Men
Aging
As men age, testosterone production often declines, and the ratio of estrogen to testosterone can shift, favoring estrogen.
Testosterone Concentrations
Serum estrogen levels in men are mediated byseveralf factors. As testosterone is the substrate for approximately 80% of serum E2, changes in serum testosterone concentrations will affect E2 levels. [1] This is why finding the best way to control estradiol on TRT is relevant.
Body Mass Index (BMI) and Obesity
Multiple studies have reported higher E2 levels in obese men and a direct relationship between E2 and BMI [4].
Men with Low testosterone who are on TRT are expected to experience rises in estrogen levels. This is more pronounced in obese males who have a significant amount of fat cells that have a lot of aromatase.
Men who are obese tend to have higher estradiol levels than men of normal weight.
Vermeulen et al. determined that subcutaneous fat as measured by computed tomography in obese men aged 30–60 was significantly and strongly associated with free E2, whereas abdominal fat was not [5].
Obese men usually suffer from a metabolic syndrome which is presented with obesity, high blood pressure, high blood sugar, and high cholesterol.
Obese men with metabolic syndrome have low testosterone levels and elevated estrogen levels. They also tend to have lower Sex Hormone Binding Globin (SHBG) levels.
Given the higher density of adipose (fat cells) in obese men, which is the primary source for aromatase, obese men tend to aromatize estrogen more than the normal weight individuals, leading to more testosterone being broken down into estrogen.
Aromatase Activity and Adipose Tissue (Fat Cells)
Aromatase is mainly found in adipose tissues (the central fat deposits of the abdomen). The more central fat cells a man has the more aromatase enzyme that is present.
Role of Estrogen in Men
The Role of Estrogen in Testosterone Regulation
Estrogen provides negative feedback to the brain (hypothalamus and pituitary), signaling to reduce the production of GnRH and LH, which are necessary for natural testosterone production. High estrogen can thus suppress your body’s own T production.
GnRH and LH, are necessary for testosterone production. Estrogen can act to block the release of these signaling hormones and halt testosterone production. Therefore, monitoring and managing Estrogen levels during TRT are crucial.
High estrogen levels lead to a decrease in testosterone production.
Bone Health
Estrogen is vital for main bone health. The impact of estrogens on bone health in men is well studied. Longitudinal studies have shown that low total and bioavailable E2 levels are associated with an increased rate of bone loss, with increased risk at a threshold of 40 pmol/L [6].
Males with low E2 levels from congenital aromatase deficiency exhibited tall stature, persistent linear growth, and delayed bone age, and osteopenia/osteoporosis. [1]
Cardiovascular Health and Metabolism
Testosterone and E2 together may facilitate endothelial-dependent vasodilation and prevent atherogenesis [1].
Men with congenital aromatase deficiency exhibited symptoms of metabolic syndrome including abdominal fat accumulation and impaired insulin sensitivity. [1]
Causes of Elevated Estrogens in Men
The upper limit of normal for E2 in men is not clinically defined. Laboratory reference ranges are assay dependent, but the upper bound is often stated as approximately 50 pg/mL or 160 pmol/L. [1]
Obesity
Obesity is associated with an increase in E2 [1], likely secondary to increased aromatase activity in subcutaneous and gluteal fat [5].
Interestingly, E2 was reduced in obese men 2 years after gastric bypass surgery, and SHBG was increased, resulting in an even greater decrease in bioavailable E2 [1].
Antiepileptic Drugs
Antiepileptic drugs, such as phenytoin and carbamazepineof, are associated with high E2 levels in men with sexual dysfunction [1]. It has been suggested that this is secondary to increased aromatase activity.
Elevated Estrogen Levels and Testosterone Deficiency
Administration of exogenous estrogen at pharmacologic doses and, in rare cases, estrogen hypersecretion from adrenal tumors are known to down-regulate testosterone through gonadotropin suppression [1].
Anabolic Steroids
Administration of Anabolic Steroids that do interact with the Aromatase enzyme can lead to great elevations of Estrogen in the body.
Symptoms of High Estrogen in Men on TRT
- Fat gain around the stomach
- Puffy ankles (look for sock marks)
- Puffy or sensitive nipples
- Unexplained emotions (sad, crying, etc)
- Erectile dysfunction
Managing High Estradiol on TRT: Finding the Best Way
If you suspect high estrogen levels are causing issues, the first step is always discussing symptoms and getting blood work done through your prescribing doctor. Finding the best way to control estradiol on TRT is highly individual.
Lifestyle Approaches
Managing Body Fat: Since fat tissue drives aromatization, reducing excess body fat through diet and exercise is often the most effective natural estrogen blocker strategy for men.
Optimize TRT Protocol: Sometimes, adjusting the dose or frequency of TRT injections (i.e smaller, more frequent shots) can lead to more stable levels and reduce E2 peaks. Discuss this with your doctor.
Pharmaceutical Options (Use With Caution & Medical Guidance)
When lifestyle isn’t enough and symptoms persist alongside confirmed high E2 levels, medications might be the next step under medical supervision of course.
Aromatase Inhibitors (AIs)
AIs work by blocking the aromatase enzyme, directly reducing the conversion of testosterone to estrogen. They are potent estrogen blocker agents.
One of the most famous and commonly discussed non-steroidal AI is Anastrozole also known as Armidex. The use of anastrozole for men on TRT is frequent in some circles but should be approached cautiously. It effectively lowers E2 but can also crash levels too low if not dosed carefully, leading to negative side effects (joint pain, low libido, poor bone health).

You can find Anastrozole through various reputable suppliers online, I recommend you answering your question “where to buy anastrozole” with Anastrozole by Swiss Chems, which is one of the most reputable suppliers currently in the market.
You can buy from our #1 choice Swiss Chems from here: [BUY NOW]
Important note: Routine AI use with TRT is generally not recommended by mainstream medical guidelines unless clear symptoms and significantly elevated E2 levels are present.
Over-suppression of estrogen is detrimental, so always consult your healthcare physician and make sure you are well studied about what you’re doing.
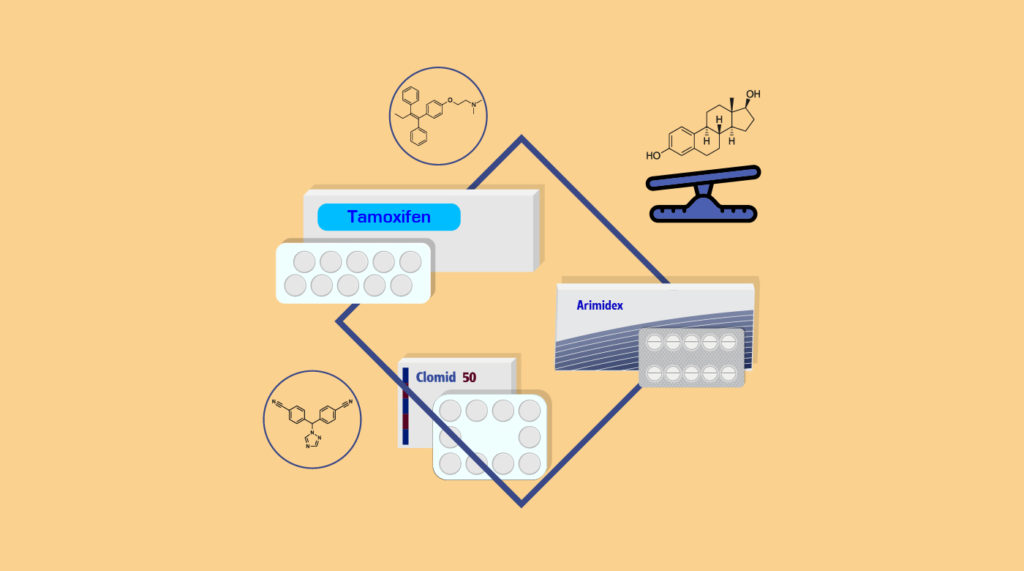
The use of aromatase inhibitors such as Arimidex or Anastrozole can stop the breakdown of testosterone.
Anastrozole is an aromatase inhibitor. Aromatase acts upon testosterone and breaks it down by a process called aromatization into estradiol. The aromatase enzyme has been found to be present in the testicles, brain, fat tissue, muscle, hair, and vascular tissues.
Many clinicians prescribed Arimidex by TRT to reduce the breakdown of testosterone and eventually reduce estrogen production and as a treatment for gynecomastia.
Aromatase inhibitors such as Arimidex can be used in men with elevated estrogen levels for the primary treatment of hypogonadism and increase testosterone levels without impairing fertility.
Aromatase inhibitors are classified into two categories, either steroidal and non-steroidal and by generation (first, second and third generations).
Steroidal aromatase inhibitors are commonly not utilized in men on TRT. Steroidal aromatase inhibitors bind to aromatase strongly (irreversibly).
Non-steroidal aromatase inhibitors, such as Anastrozole (Arimidex) reversibly bind to aromatase. Arimidex is a third-generation Aromatase inhibitors.
While Arimidex is known to reduce estrogen in men by inhibiting aromatase. It can also increase testosterone production.
Unlike TRT, patients who use Arimidex as monotherapy do not experience an increase in hematocrit and hemoglobin levels or an elevation in prostate-specific antigen (PSA).
Selective Estrogen Receptor Modulators (SERMs)
SERMs don’t lower overall estrogen levels like AIs.
Instead, they selectively block estrogen receptors in specific tissues (like the breast) while potentially acting like estrogen in others (like bone). They aren’t typically the first-line estrogen blocker for men aiming to lower systemic E2, but are used for specific issues like gyno.
Tamoxifen and Clomiphene are classified as selective ER modulators (SERMs). The SERMs and their metabolites modulate ER activation by inducing conformation changes to the ER and selectively altering signal transduction. [1]

Tamoxifen (Nolvadex) is often used to treat or prevent gynecomastia by blocking estrogen effects at the breast tissue.
Elevated estrogen levels can stimulate male breast enlargement (gynecomastia). Tamoxifen or Nolvadex has and can be used in men on TRT who experience gynecomastia, as it will block estrogen at the breast tissue.
Tamoxifen can decrease bone turnover and increase bone mineral density. [1]
Tamoxifen has also been shown to raise testosterone levels and may be effective in the treatment of male infertility. [1]
As for answering where to buy Tamoxifen online, I’ve got you covered.
You can buy Tamoxifen from our #1 choice Swiss Chems from here: [BUY NOW]
Another alternative is Clomiphene Citrate (Clomid) which is primarily used off-label to stimulate the body’s own testosterone production by blocking estrogen feedback at the pituitary [7, 9]. Not typically used alongside TRT for E2 control.

Clomiphene citrate or Clomid is a selective estrogen receptor modulator particularly when maintenance of fertility is desired, as treatment does not reduce gonadotropins or sperm concentration. [1]
It has been primarily used for infertility treatment in both genders for over 50 years. [7]
It selectively blocks estrogen receptors in the hypothalamus and pituitary, thereby increasing gonadotropin-releasing hormone, luteinizing hormone, and follicle-stimulating hormone release. This boosts endogenous testosterone levels. [7]
A previous study reported that clomiphene achieved testosterone levels comparable to those of testosterone gels. [8]
Other studies have shown improvement in erectile function with clomiphene citrate in men with secondary testosterone deficiency [10] and a recent nonrandomized study showed similar improvement in ADAM scores with clomiphene citrate compared with topical TTh [11].
Another study found that clomiphene significantly increased testosterone levels without changing prostate-specific antigen or hematocrit values. [9]
Clomiphene is a less expensive alternative to testosterone replacement with the added benefit on fertility. [7]
You can buy Clomiphene (Clomid) from our #1 supplier Swiss Chems: [BUY NOW]
Natural Support Options for Estradiol on TRT
While less potent than pharmaceuticals, some supplements are researched for potential estrogen balance support:
DIM (Diindolylmethane): Found in cruciferous vegetables, DIM may help promote healthier estrogen metabolism.
You can buy DIM (Diindolylmethane) from one of the best suppliers Thorne: [BUY NOW]
Calcium: May support the body’s process of eliminating excess estrogen.
You can buy Calcium from one of our trusted suppliers Thorne: [BUY NOW]
Zinc: Adequate zinc levels are very important for overall hormonal balance. So it’s best to supplement with Zinc if possible, especially as you age.
You can buy Zinc from one of our trusted suppliers Thorne: [BUY NOW]
Estrogen Response To TRT
The response of estrogen to TRT was studied by Lakshman et al. In a group of young men and another group of older men. [1]
Both total and free E2 levels increased with TRT. There was a higher rate of aromatization in the group of older men which was explained by greater fat mass [1].
These results suggest that in Testosterone-deficient men, TRT increases serum E2, possibly with greater increases in older or obese men. [1]
Men who are receiving injectable TRT such as testosterone cypionate or testosterone enanthate will have a higher rise in estradiol levels than other testosterone formulations.
Elevated E2 During TRT: To Treat or Not To Treat?
TRT may lead to elevations in serum E2 and some cases to levels above the upper limit of normal. [1]
The development of nipple or breast tenderness or frank gynecomastia has been reported in association with TRT. [1]
In these cases, there is a clear indication for the use of aromatase inhibitors to reduce E2. Some authors recommend withdrawal first of TRT with subsequent resolution of symptoms, followed by the use of aromatase inhibitors together with reinitiation of TTh [1].
Some clinicians, particularly in the antiaging community, advocate the routine use of aromatase inhibitors with TRT even in the absence of symptoms of estrogen excess. [1]
These clinicians believe that maintaining a relatively low estrogen concentration improves male health and the efficacy of TRT. [1]
Conclusion
There is some evidence that estrogens may contribute to the persistence of sexually stimulated erectile function when serum testosterone is severely depressed, such as in men who have undergone castration for advanced prostate cancer men.
It does not appear that naturally occurring elevations in E2 are harmful concerning testosterone levels or sexual function. E2 may increase during TRT, but elevations above the normal range are uncommon.
Elevations in E2 may resolve with prolonged TRT.
Symptoms of estrogen excess, such as gynecomastia or nipple tenderness, are rare. Men who experience such symptoms should consider temporary or permanent discontinuation of TRT, or the addition of an aromatase inhibitor.
We do not recommend the routine use of aromatase inhibitors with TRT. In the absence of signs of estrogen excess, we also find no reason to recommend the use of aromatase inhibitors in men who experience positive benefits from TTh despite elevated or high-normal E2 concentrations.
When an aromatase inhibitor is used, it should be titrated so that E2 levels remain above 40 pmol/L to preserve bone health, and monitoring of bone mineral density with DXA is recommended.
Frequently Asked Questions (FAQs)
What are the most common symptoms of high estradiol on TRT?
While individual responses vary, common signs might include increased water retention, nipple sensitivity/tenderness, increased emotionality, or sometimes reduced libido or ED (though low T is often the culprit here).
Should I use an AI prophylactically (preventatively) when starting TRT?
Most medical guidelines advise against this. It’s generally better to monitor symptoms and blood work first, and only consider an AI if necessary and under medical supervision, as crashing estrogen is detrimental.
What’s the difference between an AI and a SERM for estrogen control?
AIs (like Anastrozole) lower overall estrogen production by blocking the aromatase enzyme. SERMs (like Tamoxifen) block estrogen receptors in specific tissues (like the breast) but don’t lower total estrogen levels.
How often should I get my estradiol levels checked on TRT?
This depends on your doctor’s protocol, but typically checks are done alongside testosterone levels, perhaps initially after starting or changing dose, and then periodically (e.g., every 6-12 months) once stable.
Can losing body fat help lower my estradiol on TRT?
Yes, significantly. Since fat tissue is a primary site of aromatization (testosterone converting to estrogen), reducing excess body fat can naturally lower estrogen levels and may reduce or eliminate the need for an estrogen blocker for men.
Skip Ahead
Toggle