Recent advancements in medicine and technology have allowed for an impressive lifespan extension in the developed countries [1]. In the United States, the number of adults over 65 years of age is expected to double from 46 million to nearly 100 million by 2050.
According to the US Census Bureau, the ratio of men to women over 65 has significantly changed over the past twenty years from 67 older men per 100 older women in 1990 to the current rate of 79 older men per 100 older women. This ratio is expected to be 82 older men per 100 older women by 2030.
What Is Testosterone?
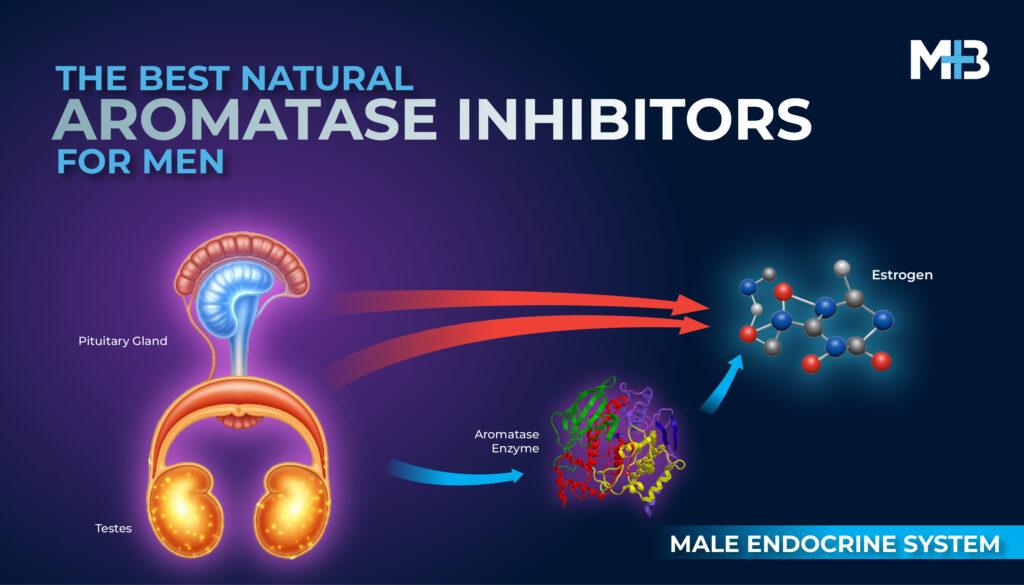
Testosterone is an essential, vital sex hormone for males, required for differentiation, developmental growth, and phenotype maintenance [1]. The levels of testosterone are regulated by the hypothalamic-pituitary-gonadal axis [1].
Every 90 min, the hypothalamic pulse generator secretes gonadotropin-releasing hormone (GnRH) into the hypothalamic-pituitary system, with subsequent release of luteinizing hormone (LH), which in turn stimulates the Leydig cells in the testes to produce testosterone [1].
Only about 2% of total testosterone circulates in the free form, while the remaining 98% is tightly bound to sex hormone binding globulin or albumin. Albumin binding is weak, and most of that fraction of testosterone is eventually bioavailable and can be measured and reported as bioavailable testosterone.
Normal Testosterone Levels and Aging
In young, healthy men (20 – 30 years old), the normal levels of serum testosterone (400 – 700 ng/dL) are controlled by the feedforward and feedback components of the hypothalamic-pituitary-gonadal axis and are maintained within the normal range of 300–800 ng/dL [1].
Several studies have shown that Serum testosterone levels decline gradually with age in men after the third decade of life at an approximate rate of 1-2% per year, varying from one to another, and are affected by several factors such as adiposity and chronic diseases [1].
Trends in Testosterone Replacement Therapy Prescription
Previous studies have shown that the declining function in older men is related to bioavailable testosterone levels. Therefore, Testosterone replacement therapy (TRT) is proposed as an intervention to improve the health span of older men.
Testosterone is currently approved by the Food and Drug Administration (FDA) for primary or secondary hypogonadism. With the worldwide increase in men’s life expectancy and the development of proper testosterone preparations, the interest in prescribing TRT has dramatically increased.
In the United States, the trend for prescribing TRT for men over 60 years of age has increased, from 1.32% in 2001 to 3.75% in 2011. A previous market analysis reported that prescription sales of TRT have increased from $150 million in 2000 to $1.8 billion in 2011 worldwide, with the United States and Canada leading the growth in sales numbers [2].
If you are diagnosed with low testosterone levels, your physician may prescribe you TRT. Despite the proven efficacy of TRT, many patients are still hesitant about seeking treatment. There are several reasons behind this hesitancy, such as outdated information, possible side effects, and being pricy.
All studies evaluating TRT prescription trends in the United States showed an increase of 1.8-4-fold over the last twenty years. Between 2000 and 2011, there was a 4.3-fold increase in testosterone testing versus a 3.7-fold rise in TRT prescriptions [2].
Who Would Need TRT?
Late-onset hypogonadism (LOH) is common in aging men and is associated with testosterone deficiency. TRT aims to improve symptoms and signs of testosterone deficiency, such as:
- Anemia.
- Depressed mood.
- Erectile dysfunction.
- Decreased libido and sexual desire.
- Reduced muscle mass and strength.
- Reduced bone mass and osteoporosis.
- Insomnia and a reduced sense of general well-being.
- Forgetfulness, difficulty in concentration, and loss of memory
How Much Does TRT Cost?
To answer this question, let’s break down the costs according to what treatment usually entails.
Blood Work and Laboratory Evaluation

Sex hormone binding globulin (SHBG) accounts for 60% of testosterone binding, while the remaining 40% of the total testosterone is bound by albumin or other proteins. Bioavailable testosterone – free and albumin-bound testosterone – is thought to reflect an individual’s biologically active, circulating testosterone.
Biochemical markers commonly used to assess testosterone deficiency include total testosterone, free testosterone, calculated free testosterone, bioavailable testosterone, and free androgen index. SHBG levels should be evaluated in symptomatic patients with borderline total testosterone, especially in obese or older men.
The diagnosis of testosterone deficiency should be made only after taking two total testosterone measurements on separate occasions between 8, and 11 am due to the circadian rhythm of testosterone production by the testicles [3]. In 2018, the American Urological Association recommended the use of TRT in patients with total testosterone < 300 ng/dl [3].
In patients with low testosterone, serum LH should be measured to establish the etiology of testosterone deficiency. Serum prolactin levels should be measured in patients with low testosterone levels combined with low serum LH levels to screen for hyperprolactinemia. Elevated prolactin levels can indicate the presence of pituitary tumors, such as prolactinomas [4].
The cost of blood work to diagnose testosterone deficiency, including a complete, specific hormone panel, can cost as much as $800 – $1,500. If you opt for an at-home test, a total testosterone test may cost $50 – $70.
Meet with a Specialist
Your lab results returned, and your total testosterone was < 300 ng/dl. What’s next? Now, schedule your appointment with a urologist, endocrinologist, or internist. Your physician will review your medical history and tailor a treatment plan that fits your clinical presentation. This appointment will cost you about $45.
TRT Preparations and Monthly Costs
Oral Preparation
Oral preparations come with a high risk of liver toxicity and lack of inability to induce virilization in most patients.[5] Therefore, it’s not the best option. Testosterone tablets can be a very costly alternative – anywhere from $100 to $300 a month.
Long-acting Intramuscular Injections
Long-acting intramuscular injections of testosterone esters have been used for many years for the treatment of hypogonadism. The main advantages of these formulations, especially T enanthate, are the effective initiation and maintenance of normal virilization, freedom from daily administration, and low cost.[5] The drawbacks of this preparation include the need for deep intramuscular injection every 1–3 weeks and fluctuations in serum testosterone levels resulting in fluctuations in energy, mood, and libido in many patients.[5]
Extra-long-acting Injections
An extra-long-acting injection is also available in Europe and the United States containing T undecanoate in oil.[6] The prolonged duration of action (half-life of 34 days in castor oil) allows for increased dosing intervals. The main advantages are achieving relatively stable normal testosterone levels and less frequent dosages. Disadvantages include the rather long wash-out period, which may be challenging if complications appear, higher cost than other IM formulas, and the risk of pulmonary oil microembolism and anaphylaxis.[5] Therefore, monitoring of the patient for 30 min post-injection is recommended.
In general, Injections are the most affordable TRT option. Without insurance coverage, the cost of a single 200 mg/mL testosterone vial can range between $40 and $100 a month.
Transdermal Preparation
Transdermal T preparations such as patches, gels, or solution. Their pharmacokinetic profile mimics the physiological diurnal variations of testosterone concentration[7], easy to eliminate upon removal in case of adverse effect due to its short duration of action. Advantages include achieving relatively stable testosterone levels. However, in some hypogonadal patients, normal serum testosterone levels cannot be reached, especially in patients with high body mass index (BMI), since obesity seems to affect the pharmacokinetics of transdermal preparations. Other disadvantages include the need for daily administration, relatively high cost, and skin irritation. Transdermal testosterone formulas can cost as little as $30 to $500 a month.
Subdermal Preparation
Subdermal testosterone implants also result in stable testosterone levels and have the advantage of reduced dosing frequency. However, the need for surgical incision and the limited data regarding testosterone levels during therapy make this modality less favorable than others.
Buccal Preparation
Buccal mucoadhesive testosterone tablets require twice daily application and result in even testosterone serum levels. Although, this formulation has the advantage of a quick reversal of testosterone action upon removal (2–4 h) and mimics circadian testosterone rhythm. However, it has been associated with alteration in taste and gum-related problems in 3–15% of treated patients.
Nasal Preparation
The recently approved nasal testosterone gel represents a novel non-invasive route for TRT, which also minimizes the risk of transference but has the disadvantages of frequent dosing (three times per day), intolerance in patients with underlying nasal or sinus pathology, and lack of data regarding overall efficacy and safety.
What Is the Best TRT for Me?
Overall, the choice of the appropriate TRT regimen should be a shared decision made by the physician and the patient and should consider patient preference and characteristics, convenience, cost, insurance coverage, formulation-specific pharmacokinetics, and side effects.
Does Insurance cover Testosterone Replacement Therapy?
According to Harvard Health, normal testosterone levels in young, healthy men range between 300 and 1,000 ng/dl. Most insurance companies will cover your TRT with a serum testosterone level < 300 ng/dl with two separate blood tests, usually in the morning.
Who Is Not a Candidate for TRT?
Current Guidelines Recommend Against Initiating TRT In Men With
- Known prostate cancer (locally advanced or metastatic) [8]
- Prostate nodule/induration or PSA > 4 ng/ml [8]
- Severe lower urinary tract symptoms (LUTS) with an International Prostate Symptom Score (IPSS) > 19.
- Hematocrit > 50% or > 54% according to European Association of Urology (EAU) [9]
- Untreated severe sleep apnea [8]
- Uncontrolled or poorly controlled severe heart failure [8]
- The active desire for fertility [8]
TRT may begin if LUTS, erythrocytosis, and sleep apnea are successfully treated.[5] TRT should also be considered for hypogonadal men, surgically treated for localized prostate cancer, who are currently without evidence of disease for at least two years and have a low risk for recurrence [10]
Adverse Effects of TRT
Prostate Cancer
TRT increases prostate volume and PSA. There is unequivocal evidence that TRT can stimulate growth and aggravate symptoms in men with locally advanced or metastatic prostate cancer.
Erythrocytosis
Erythrocytosis is a common adverse effect of TRT, particularly with testosterone ester injections and in older men. Middle-aged and older men on TRT are nearly four times as likely to have HCT > 50%.
Fertility
Exogenous testosterone suppresses LH secretion and thereby decreases the high intratesticular testosterone levels essential for spermatogenesis. Therefore, hypogonadal men who are being considered for TRT should be told of the suppressive effect of testosterone on spermatogenesis and asked if they desire fertility.[5]
Venous Thromboembolism
The known association between TRT and erythrocytosis and a report that demonstrated an increased risk of venous thromboembolism in men receiving TRT, especially in those with underlying thrombophilia, have led the FDA to require adding a general warning to testosterone products about the potential risk for venous blood clots.[3] Therefore, it is crucial to obtain a careful personal and family history before initiating TRT.[5]
Cardiovascular Disease
Data regarding the cardiovascular safety of TRT have been conflicting and inconclusive. The use of injectable preparations is associated with a greater risk of myocardial infarction and stroke, but not VTE, compared with T gel use.[3] However, more recent studies have shown that TRT is not associated with an increased risk of cardiovascular disease.
In general, testosterone treatment is contraindicated in men with severe HF as fluid retention may worsen the condition[10] and in patients with unstable CV disease or improve cardiac outcomes.[8]
TRT Monitoring
The patient should be evaluated for outcome improvement at 3, 6, and 12 months after initiation of treatment and then annually.[10] Serum testosterone levels should be measured 3 to 6 months after initiation of therapy or changes in the dose, and then, if stable, monitoring should be done every 6–12 months.[5]
In the case of primary hypogonadism, normalization of the serum LH concentration may be used to judge the efficiency of TRT, no matter which preparation is used.[5]
In men over 50 years of age or older than 40 years of age with baseline PSA > 0.6 ng/ml, a digital rectal examination should be performed. PSA level should be measured before initiating treatment and at 3, 6, 12 months, and annually after that or in accordance with prostate cancer screening guidelines depending on the patient’s age and race.[10]
Hematocrit (Hct) should be measured before initiating treatment, and if it is elevated, the cause should be sought before TRT is commenced. It should be re-evaluated after 3 to 6 and 12 months and annually. If Hct increases to > 54%, the patient should be evaluated for aggravating factors such as smoking and sleep apnea and TRT should be temporarily stopped and the TRT regimen tailored accordingly.[10]
Before initiating TRT, patients with pre-existing cardiovascular disease should be assessed for related symptoms. During treatment, careful monitoring is warranted, including clinical evaluation and regular measurements of Hct and serum T levels.
Skip Ahead
Toggle